What does the mental health payment system mean for people?
How many boxes can you fit people with mental health problems into?
The answer, apparently, is, 21.
Over the last five years, the way in which money flows through the mental health system has changed. To make this change, policy makers and health professionals needed a way of grouping people with mental health problems according to their needs. As a result they produced 21 "clusters" - groups, or boxes, if you will - which fall under three main headings: non-psychotic, psychotic and organic mental health conditions.
For example, cluster 4 relates to people with sever non-psychotic conditions and cluster 10 relates to people with first episode psychosis.
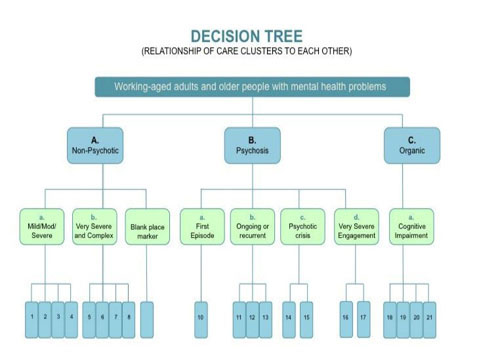
In a world that is shifting to personalised approaches and outcomes, the idea of filtering people according to one of 21 groups seems absurd. How can this be personalised?
Those proposing this way of working suggest that the new payment system can give commissioners and providers a greatly improved sense of who the people are who use services, what they want and need, and can improve people's choice in how those needs are met. The clustering process, it is argued, helps to create better assessments and pathways for people to travel along, depending on their mental health problem and their other circumstances. It also is said to mean that care pathways should be paid for flexibly and coordinated according to what individuals want, rather than having block contracts arranged mainly between commissioners and providers with little input from people who use services.
In practice, progress has yet to demonstrate these benefits. Despite having been on the agenda in mental health for over five years, and compulsory since 2012/13, surveys have found that efforts so far have had little impact on provider finances or financial arrangements, and that service users are only occasionally involved in developing the new mental health payment system.
These new payment arrangements are likely to continue to be part of the way the NHS works. So it is vital that people in their local areas become involved to help bridge the gap between theory and practice and ensure the system succeeds in helping to deliver personalised outcomes.
Over the last 18 months, NDTi has been exploring what might help. From this work, we think there are five things people can practically do at a local level to make an impact:
1. Find out who is coordinating the work to develop the new mental health payment system, and ask them what progress has been made locally. This will help bring out this work into the open - which it generally isn't.
2. Find out when, where and how regularly joint meetings take place between commissioners across health, social care and public health, as well as with providers from all sectors - and then ensure that people who use services and their families are involved in these meetings. This will help to introduce and encourage co-production in the development of the new mental health payment system
3. People using mental health services could ask their social worker, community psychiatric nurse, other care coordinator or lead professional how the clustering and assessment processes are related to each other locally. This has a double benefit: first it shows people are aware of the new payment system and, second, it provides an opportunity for them to ensure these processes are coordinated and transparent and person centred
4. Similarly, ask them what the local pathway is for each cluster, and ask about what choice and flexibility there is in accessing different parts of that pathway
5. Remember that options like Direct Payments and Personal Health Budgets remain opportunities for people to explore.
At NDTI we have created a similar list for actions that commissioners can take.
It is counterintuitive that an approach which includes putting people in one of 21 boxes could support personalised approaches and outcomes. The new mental health payment system is aiming to show this could be done - but it will not be unless a full understanding of personalisation, person centred working and co-production are part of its implementation. By understanding more about what approach is being taken locally and by getting involved, people with mental health problems have an opportunity to increase the likelihood that this work is done properly.

Comments
Add your comment